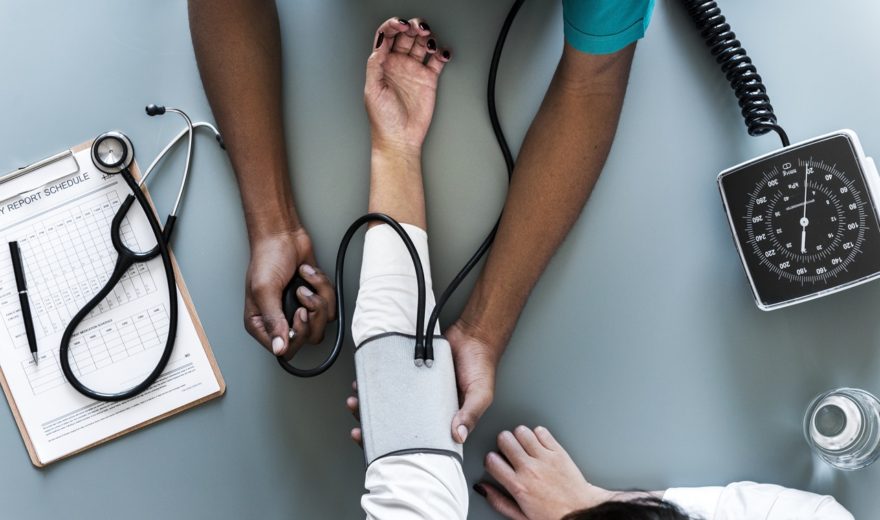
The Tax bill passed in December eliminated the individual mandate requiring consumers to have health insurance or pay a tax penalty, starting in 2019. As healthy individuals drop their insurance, it is expected that premiums will rise by an average of 20% next year for individual plans on the insurance exchange. As prices rise, this creates a negative feedback loop where more healthy people cannot afford insurance, the insurance pool becomes worse for insurers, and premiums increase again.
As a result, more consumers are adopting higher deductibles and pay for more of their care out of pocket. Health Insurance will shift from being used for every appointment to being catastrophic coverage where you will only have claims in rare years. Think of your auto insurance – you don’t expect it to pay for oil changes, only when you have a wreck.
This will shift the burden of cost-savings to the consumer rather than the insurer. Unfortunately, doctors offices and hospitals are terrible at sharing price information with patients, so it’s extremely difficult to know how much something will cost at one office, let alone be able to determine if you could save money by going elsewhere.
Cost transparency is the only thing that is going to save our health system from continuing to escalate out of control. We have a fee for service system which encourages for-profit hospitals to charge as much as they can and to add on extra tests, services, and procedures to increase their bills. And it’s not easy being a doctor, where every patient wants a quick-fix (other than eat right, exercise, and take care of your body in advance). With the risk of malpractice claims, doctors order extra tests to cover themselves even if the actual need for those tests is small. That’s called “Defensive Medicine”, and it’s not about defending the patient.
At a conference I attended last week, a Doctor turned financial advisor presented information on how to save money on your health care. Here are nine tips:
1. In-Network. Don’t ask a doctor if they take your insurance, ask “Are you in my network?”. Write down who you spoke with and the date and time. Later, if you get a bill that shows out-of-network charges, you can contest that with the evidence of what you were told. In fact many doctors offices record their calls, and you can demand to listen to your call.
2. PPOs used to offer choice of going anywhere, but networks are often very narrow for small plans. A cheap plan usually means that very few doctors are in that network. You have to ask at each step. If you have a planned hospital procedure, get a signed estimate in advance, and write on your paperwork: “I will only allow in-network care.” Otherwise, you may find out that some of your care is out of network even when you are at an in-network hospital!
3. Balance Billing. If you are out of network, you may be billed for the difference between the in-network price and what the hospital wants to charge you. For example, in Texas, insurance will pay up to $12,668 for an Appendectomy, but the average hospital bill is $40,893. So when you get an outrageous bill, you can find out this information to negotiate a lower price. This information is published by the Texas Department of Insurance Healthcare Costs Guide.
4. If you go to an in-network hospital and receive charges from an out-of network provider for over $500, you have the right to seek Medical Bill Mediation again through the Texas Department of Insurance. They have been able to lower these bills in 90% of the cases submitted to the state.
5. Reduce unnecessary tests and medications. The vast majority of a doctor’s diagnosis comes through patient history and the physical examination. Doctors today have to see a large number of patients and are in a hurry, so they often default to ordering expensive tests to save time. Before going to an appointment, type up your symptoms, medical history, medications, and diet. Write down the questions you have. Print three copies. Mail one in advance. Give one copy to the receptionist when you arrive. And if the doctor walks in without it, give them the third copy.
If they want to order additional testing, ask: What do you hope to learn from this test? How will the results of this test change the approach to treatment? If they are going to prescribe medicine, ask how long you will take the medicine. What are the benefits, side effects, and risks? What alternatives (i.e. lifestyle) are there to this medicine?
6. Independent Practice or Hospital. Hospitals are buying up doctors offices in their area and raising prices. Where a doctor might charge $100 for an office visit, a hospital can charge $250. Ask if an office is an independent practice or part of a hospital.
7. Ask your pharmacist if there are generics or less expensive substitutes for your medicines. Doctors are not always aware of the price of the medicines they prescribe.
8. If you hit your deductible during the year, try to take advantage of the fact that insurance has kicked in. Fill your prescriptions in December for the year ahead. Complete any tests that you should have done. If you’ve put off knee surgery or other procedures, try to get those done as well.
9. If you have a High Deductible Health Plan, fund your Health Savings Account (HSA), so you can pay your co-pays, deductible, prescriptions, and other costs with pre-tax money. That’s like saving 12-37% on every dollar you spend.
If you don’t have an HSA, but your employer offers a Flexible Spending Account (FSA), that will also allow you to pay medical bills with pre-tax money. Just remember that unlike an HSA, FSA is use it or lose it – money not spent before December 31 is forfeited.
Healthcare costs have increased by 7.76% a year since 1970. The US spends about 19% our GDP on healthcare each year, significantly more than any other nation. Even countries which guarantee healthcare for everyone only spend 11-13% of their GDP. We have a broken system but seem unwilling to learn from what works in other parts of the world.
The trend will continue: to reduce insurance claims, more expenses will be shifted to the consumer. Capitalism works to bring down costs, but it requires that consumers have price transparency, something which doctors and hospitals have been unwilling to do. They should publish their prices and post prices on their website. Today, we have to ask and be our own advocate to keep healthcare costs down.